Healthcare Payer Services Market Size, Share and Trends Analysis 2026 to 2035
What is Healthcare Payer Services Market Size?
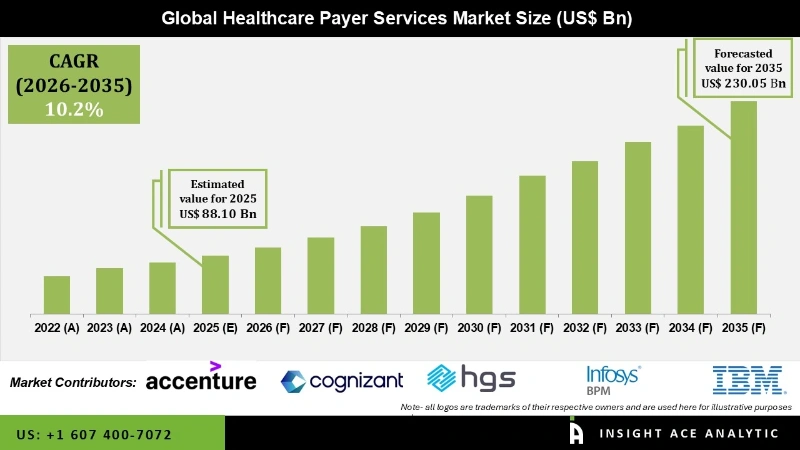
Global Healthcare Payer Services Market Size is valued at USD 88.10 Billion in 2025 and is predicted to reach USD 230.05 Billion by the year 2035 at a 10.2% CAGR during the forecast period for 2026 to 2035.
Healthcare Payer Services Market Size, Share & Trends Analysis Report By Services (BPO Services, ITO Services, KPO Services), By Application (Claims Management Services, Integrated Front Office Service & Back Office Operations, Member Management Services, Provider Management Services, Billing & Accounts Management Services), By End Use, By Region, And Segment Forecasts, 2026 to 2035.
Healthcare Payer Services Market Key Takeaways:
|
Key Industry Insights & Findings from the Report:
- The industry is driven by rising consumer spending on healthcare and substantial infrastructure upgrades, particularly in developing nations.
- Growing insurance enrollment, an increase in healthcare fraud, and a rise in the application of healthcare analytics are projected to propel the market for healthcare payer solutions.
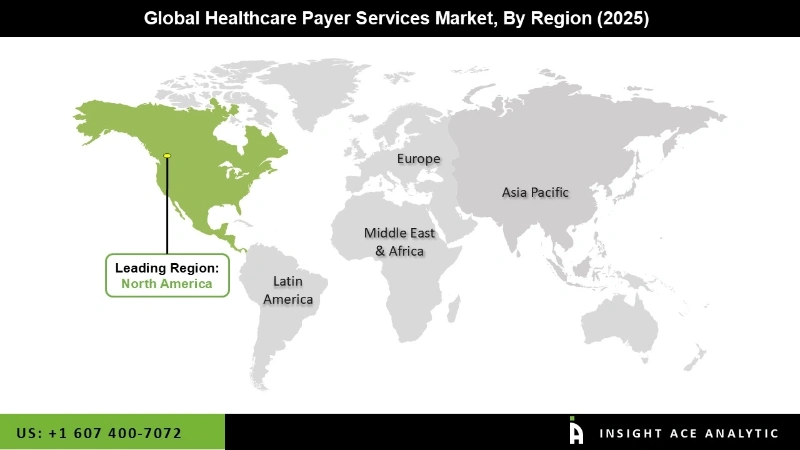
- North America dominated the market and accounted for a revenue share of global revenue in 2025.
- The growth of the market is expected to be limited by management control loss, linguistic and cultural barriers, and expensive outsourcing.
Healthcare supply chain business process outsourcing is contracting out the healthcare supply chain administration to outside service providers (BPO). The demand for improved supply chain management (SCM) techniques and the increase in the necessity for cost-effective operations are factors contributing to this industry's growth. Over the projected period, reducing the overall cost of healthcare supply chain BPO services is predicted to fuel market expansion.
Also, the need for healthcare supply chain business process outsourcing is growing due to inventory management, and the market is anticipated to expand throughout the forecast period as a result. The use of ICD-10 codes, a drop in the cost of healthcare delivery, and other reasons are also expediting the growth of the healthcare supply chain BPO industry.
Healthcare payers had difficulties as a result of the COVID-19 pandemic, and some health insurers fared better financially during the epidemic due to reduced healthcare funding. Healthcare providers have received strong assistance from the payers. They have established community programs for health equity, broadened eligibility to allow patients to keep their medical treatments, provided advance payments, and constructed web portals that deliver quick and accurate information about the epidemic. The important parties are forming strategic alliances for initiatives addressing systemic health disparities.
Recent Developments:
-
In March 2024, Oracle has recently made important improvements to Oracle Health Data Intelligence, including the addition of a new generative AI service designed to boost the efficiency of care management. Oracle Health Data Intelligence, formerly referred to as HealtheIntent, was a collection of cloud-based applications, services, and analytics that were organized in a modular manner. The system was enhanced with additional capabilities, such as improved system performance, pre-built clinical quality analytics, and automatic alarms. These enhancements resulted in more reimbursements and improved care.
-
In May 2022, Omega Healthcare has declared the procurement of ApexonHealth, Vasta Global, and Reventics as a component of its plan to expedite the organization's progression. Omega Healthcare utilized strategic acquisitions to expand its AI and data-analytics-driven solutions, enabling healthcare clients to optimize revenue and save costs by leveraging big data and automation technology. Omega Healthcare enhanced its current Clinical Documentation Improvement (CDI) capabilities by implementing technology-driven solutions. Additionally, the company increased its core coding and Revenue Cycle Management (RCM) services.
Competitive Landscape:
Some of the Healthcare Payer Services market players are:
- Accenture
- Allscripts Healthcare, LLC
- Cognizant
- Concentric Corporation
- Conduent, Inc.
- Conifer Health Solutions, Llc
- Dell Inc.
- Exl
- Firstsource Solutions
- Genpact Limited
- Hcl Technologies Limited
- HGS Ltd.
- IBM
- Infosys Bpm
- Inovalon
- IQVIA Inc.
- Mphasis
- NTT Data Corporation
- Omega Healthcare
- Oracle Corporation
- Parexel International Corporation
- R1RCM, Inc.
- Sas Institute, Inc.
- Tata Consultancy Services
- Unitedhealth Group
- Wipro Limited
- WNS (Holdings) Ltd.
- Xerox Corporation
Market Segmentation:
The Healthcare Payer Services market is segmented by service, application, and end-use. Based on service, the market is segmented into BPO Services, ITO Services, and KPO Services. By the application, the market is segmented into Claims Management Services, Integrated Front Office Service & Back Office Operations, Member Management Services, Provider Management Services, Billing & Accounts Management Services, Analytics & Fraud Management Services, and HR Services. By end-use, the market is segmented into Private and Public Payers.
Based On Service, The KPO Segment Is Accounted As A Major Contributor In The Healthcare Payer Services Market
Due to the spike in demand for highly qualified workers and the cost-benefit associated with outsourcing high-end activities at a cheap cost to emerging countries, the healthcare payer KPO category is predicted to grow at a profitable CAGR. In addition, one of the key factors projected to fuel the sector's growth in the upcoming years is the growing demand in emerging nations for low-cost, highly qualified personnel for domain-specific core and non-core operations of the payer vertical.
The Claims Management Services Segment Witnessed Growth At A Rapid Rate
Claims management services held the primary stake. Among other important factors that are influencing the number of people enrolled in the Centers for Medicare and Medicaid Services are the existence of the Affordable Care Act and rising overall healthcare spending. The majority of a payer's burden is made up of claims processing services, which are the most data-intensive operations. The providers' claims are examined for compliance with eligibility requirements, veracity, and the precise amount that needs to be reimbursed. The process has been streamlined, and turnaround times have greatly increased as a result of the advent of the digital era.
The North America, Healthcare Payer Services Market, Holds A Significant Revenue Share In The Region.
The market was dominated by North America. The need for healthcare supply chain business process outsourcing is expected to develop during the forecast period due to the rising demand for healthcare IT services. The demand for healthcare supply chain business process outsourcing is projected to rise as a result of evolving regulatory environments and mounting pressure on the healthcare sector to reduce service costs. Thus, during the projection period, the regional market is anticipated to experience significant expansion.
Healthcare Payer Services Market Report Scope:
| Report Attribute | Specifications |
| Market size value in 2025 | USD 88.10 Billion |
| Revenue forecast in 2035 | USD 230.05 Billion |
| Growth rate CAGR | CAGR of 10.2% from 2026 to 2035 |
| Quantitative units | Representation of revenue in US$ Mn, and CAGR from 2026 to 2035 |
| Historic Year | 2022 to 2024 |
| Forecast Year | 2026-2035 |
| Report coverage | The forecast of revenue, the position of the company, the competitive market statistics, growth prospects, and trends |
| Segments covered | Service, Application, and End-Use |
| Regional scope | North America; Europe; Asia Pacific; Latin America; Middle East & Africa |
| Country scope | U.S.; Canada; U.K.; Germany; China; India; Japan; Brazil; Mexico; The UK; France; Italy; Spain; China; Japan; India; South Korea; Southeast Asia; South Korea; Southeast Asia |
| Competitive Landscape | Cognizant; EXL; HGS Ltd.; Accenture; Xerox Corporation; Concentric Corporation; Genpact; WIPRO Ltd.; HCL Technologies |
| Customization scope | Free customization report with the procurement of the report, Modifications to the regional and segment scope. Particular Geographic competitive landscape. |
| Pricing and available payment methods | Explore pricing alternatives that are customized to your particular study requirements. |
Segmentation of Healthcare Payer Services Market-
Healthcare Payer Services Market By Service-
- BPO Services
- ITO Services
- KPO Services
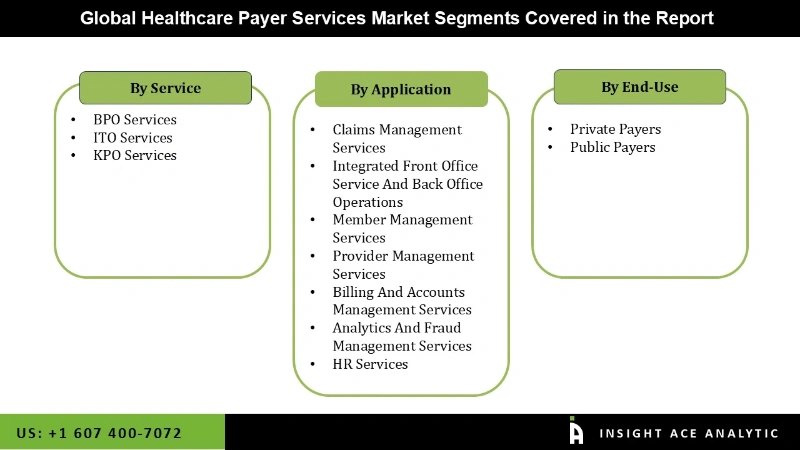
Healthcare Payer Services Market By Application-
- Claims Management Services
- Integrated Front Office Service And Back Office Operations
- Member Management Services
- Provider Management Services
- Billing And Accounts Management Services
- Analytics And Fraud Management Services
- HR Services
Healthcare Payer Services Market By End Use-
- Private Payers
- Public Payers
Healthcare Payer Services Market By Region-
North America-
- The US
- Canada
Europe-
- Germany
- The UK
- France
- Italy
- Spain
- Rest of Europe
Asia-Pacific-
- China
- Japan
- India
- South Korea
- South East Asia
- Rest of Asia Pacific
Latin America-
- Brazil
- Mexico
- Argentina
- Rest of Latin America
Middle East & Africa-
- GCC Countries
- South Africa
- Rest of Middle East and Africa
Research Design and Approach
This study employed a multi-step, mixed-method research approach that integrates:
- Secondary research
- Primary research
- Data triangulation
- Hybrid top-down and bottom-up modelling
- Forecasting and scenario analysis
This approach ensures a balanced and validated understanding of both macro- and micro-level market factors influencing the market.
Secondary Research
Secondary research for this study involved the collection, review, and analysis of publicly available and paid data sources to build the initial fact base, understand historical market behaviour, identify data gaps, and refine the hypotheses for primary research.
Sources Consulted
Secondary data for the market study was gathered from multiple credible sources, including:
- Government databases, regulatory bodies, and public institutions
- International organizations (WHO, OECD, IMF, World Bank, etc.)
- Commercial and paid databases
- Industry associations, trade publications, and technical journals
- Company annual reports, investor presentations, press releases, and SEC filings
- Academic research papers, patents, and scientific literature
- Previous market research publications and syndicated reports
These sources were used to compile historical data, market volumes/prices, industry trends, technological developments, and competitive insights.
Primary Research
Primary research was conducted to validate secondary data, understand real-time market dynamics, capture price points and adoption trends, and verify the assumptions used in the market modelling.
Stakeholders Interviewed
Primary interviews for this study involved:
- Manufacturers and suppliers in the market value chain
- Distributors, channel partners, and integrators
- End-users / customers (e.g., hospitals, labs, enterprises, consumers, etc., depending on the market)
- Industry experts, technology specialists, consultants, and regulatory professionals
- Senior executives (CEOs, CTOs, VPs, Directors) and product managers
Interview Process
Interviews were conducted via:
- Structured and semi-structured questionnaires
- Telephonic and video interactions
- Email correspondences
- Expert consultation sessions
Primary insights were incorporated into demand modelling, pricing analysis, technology evaluation, and market share estimation.
Data Processing, Normalization, and Validation
All collected data were processed and normalized to ensure consistency and comparability across regions and time frames.
The data validation process included:
- Standardization of units (currency conversions, volume units, inflation adjustments)
- Cross-verification of data points across multiple secondary sources
- Normalization of inconsistent datasets
- Identification and resolution of data gaps
- Outlier detection and removal through algorithmic and manual checks
- Plausibility and coherence checks across segments and geographies
This ensured that the dataset used for modelling was clean, robust, and reliable.
Market Size Estimation and Data Triangulation
Bottom-Up Approach
The bottom-up approach involved aggregating segment-level data, such as:
- Company revenues
- Product-level sales
- Installed base/usage volumes
- Adoption and penetration rates
- Pricing analysis
This method was primarily used when detailed micro-level market data were available.
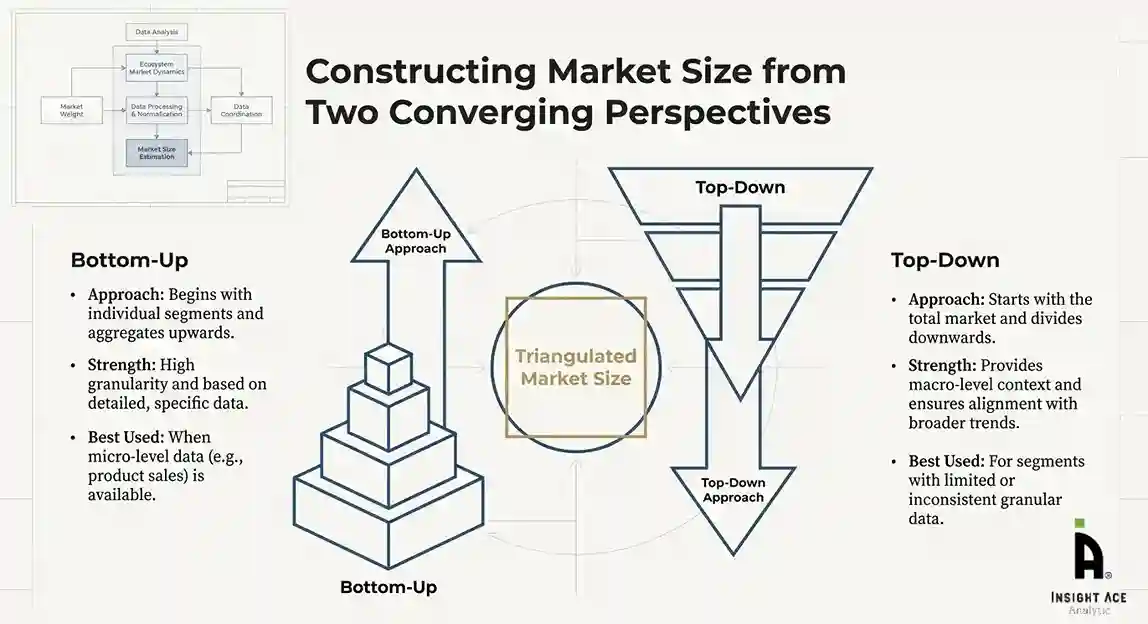
Top-Down Approach
The top-down approach used macro-level indicators:
- Parent market benchmarks
- Global/regional industry trends
- Economic indicators (GDP, demographics, spending patterns)
- Penetration and usage ratios
This approach was used for segments where granular data were limited or inconsistent.
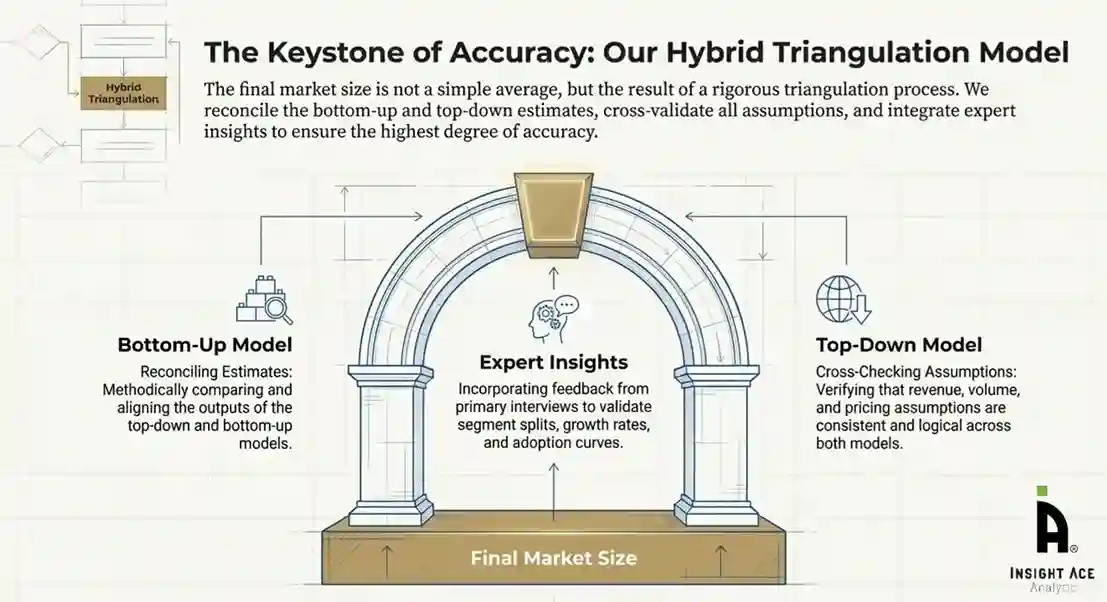
Hybrid Triangulation Approach
To ensure accuracy, a triangulated hybrid model was used. This included:
- Reconciling top-down and bottom-up estimates
- Cross-checking revenues, volumes, and pricing assumptions
- Incorporating expert insights to validate segment splits and adoption rates
This multi-angle validation yielded the final market size.
Forecasting Framework and Scenario Modelling
Market forecasts were developed using a combination of time-series modelling, adoption curve analysis, and driver-based forecasting tools.
Forecasting Methods
- Time-series modelling
- S-curve and diffusion models (for emerging technologies)
- Driver-based forecasting (GDP, disposable income, adoption rates, regulatory changes)
- Price elasticity models
- Market maturity and lifecycle-based projections
Scenario Analysis
Given inherent uncertainties, three scenarios were constructed:
- Base-Case Scenario: Expected trajectory under current conditions
- Optimistic Scenario: High adoption, favourable regulation, strong economic tailwinds
- Conservative Scenario: Slow adoption, regulatory delays, economic constraints
Sensitivity testing was conducted on key variables, including pricing, demand elasticity, and regional adoption.
Request Customization
Add countries, segments, company profiles, or extend forecast — free 10% customization with purchase.
Customize This Report →Enquire Before Buying
Speak with our analyst team about scope, methodology, pricing, or deliverable formats.
Enquire Now →Frequently Asked Questions
Healthcare Payer Services Market Size is valued at USD 88.10 Billion in 2025 and is predicted to reach USD 230.05 Billion by the year 2035.
Global Healthcare Payer Services Market expected to grow at a 10.2% CAGR during the forecast period for 2026-2035.
Cognizant; EXL; HGS Ltd.; Accenture; Xerox Corporation; Concentric Corporation; Genpact; WIPRO Ltd.; HCL Technologies
Healthcare Payer Services market is segmented by service, application, and end-use, Services, Integrated Front Office Service & Back Office Operations, Member Management Services, Provider Management Services, Billing & Accounts Management Services, Analytics & Fraud Management Services, and HR Services.
North America region is leading the Healthcare Payer Services Market.